Healthcare Contract Management Platform: How Automation Beats An Internal Contract Manager
.svg)
.svg)
Providers often come to us once they’ve realized that a healthcare contract management platform helps stop revenue leaking via denials, underpayments, and weak patient collections. They’re tired of their reactive strategies: denial appeals, underpayment notifications, and the hounding of patients for monies owed. Those tactics take more effort and cost on the back end than preventing them on the front end would.
There are several ways to get contracts under control: outsourcing to a third party (expensive), bringing in an internal contract manager, or using the automation that comes with a healthcare contract management platform.
Here, we review the advantages and pitfalls of hiring internally or using a contract management platform. Your choice depends on your organization’s structure and current challenges, but you need to know the advantages and limits of both.
What Is a healthcare contract management platform?
A healthcare contract management platform is a comprehensive software solution designed to streamline and optimize the entire lifecycle of contracts within healthcare organizations.
It automates tasks such as contract creation, negotiation, execution, and renewal, ensuring that all agreements are properly tracked and managed. By providing a centralized repository for storing and accessing contracts, staff can more easily locate specific documents and monitor compliance with regulatory requirements. Built on advanced technologies like artificial intelligence and machine learning, these platforms can analyze contract data to identify potential risks, opportunities for cost savings, and areas for improvement in contract terms.
Healthcare contract management platforms help ensure that all stakeholders are aligned and informed about contractual commitments by providing real-time visibility into contract performance and obligations. Additionally, these platforms often integrate with existing systems, such as revenue cycle management and electronic health records, to create a seamless workflow. By revealing which payers provide the most contractually accurate reimbursements, keep denials reasonable, and respond to requests in a timely manner, healthcare contract management platforms help organizations manage complex contractual relationships with payers.
Take a quick, self-guided tour through a powerful contract management and underpayments identification tool:
Healthcare Contract Management Platform v. Internal Contract Manager Breakdown
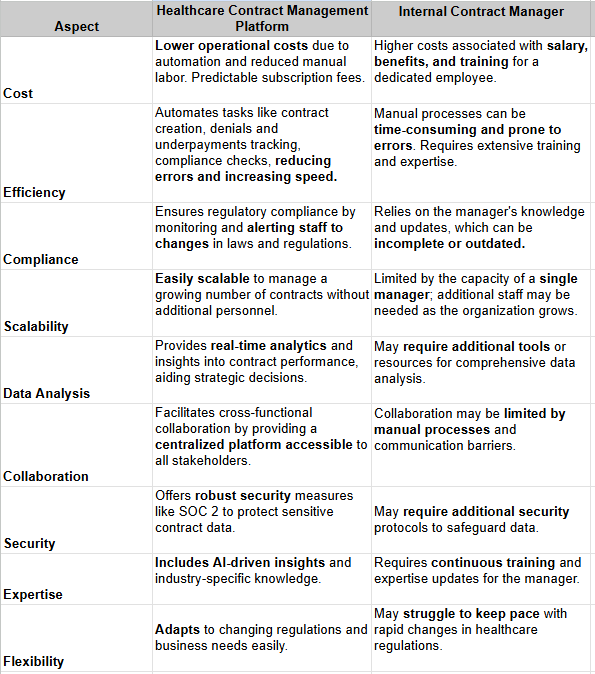
Advantages of automated healthcare contract management platforms
While employing an internal contract manager can provide some benefits, leveraging healthcare contract management software offers a comprehensive, more affordable and efficient solution. Here are the areas where automation surpasses using an internal healthcare contract specialist:
1. Cost savings and revenue optimization
- Data-driven negotiations: Software provides fast, real-time insights into contract terms and performance, enabling healthcare providers to negotiate better rates and identify underperforming contracts. Our payer contract negotiation article covers how providers can establish a strong negotiation as well as recognize the tricky terms payers use to nudge monies in their direction. It could take an individual contract specialist a week and internal or external data analysts to calculate the performance of all payers and create a dashboard comparing them.
Comprehensive contract analysis also cranks out the data that healthcare providers can use to ground their contract negotiation strategies. By meticulously examining actual vs. contracted reimbursements, denials, payer timeliness that the healthcare contract management platform delivers with a few keystrokes, organizations can construct a compelling argument for enhanced contract conditions.
- Reduced Operational Costs: Automation reduces administrative overhead and minimizes the need for extensive manual labor, resulting in cost savings. A Black Book survey of 1,302 hospital financial executives reveals that participants using revenue cycle software platforms achieve a 27% decrease in the cost of collecting and increased net patient revenue of 6%.
On the other hand, the internal healthcare payer contract manager often relies on staff from various departments for support in their work. They work with financial and operational staff as well as legal teams. In addition, they’ll need data analysts to provide insights into contract performance.
2. Scalability and adaptability
- Future-proofing: As healthcare technology and regulations evolve, automated contract management systems can more easily ingest and share new requirements, ensuring ongoing compliance and efficiency. It would take an internal contract manager constant tracking of payer portals, newsfeeds, and government agencies to stay up to date on every change. Granted, some do come into the organization. The contract manager then has to upload that information into their contract management platform one by one.
- Integration capabilities: Healthcare contract management platforms integrate with existing operational tools, creating a seamless workflow and supporting the organization's growth.
2. Enhanced efficiency and productivity
- Automated workflows: Contract management software automates tedious tasks such as contract creation, eligibility verification, review and tracking, reducing manual workload and minimizing errors. The robust platforms can also delegate denials and underpayments to staff members determined by parameters created during integration. This way, staff can start their day with a list of work to attend to, avoiding the need to come up with their priorities themselves.
- Centralized repository: A digital platform provides a centralized storage system for contracts, making them easily accessible and searchable for all involved, which is often challenging with manual systems.
4. Improved compliance and risk mitigation
- Regulatory compliance: Automated systems ensure compliance with healthcare regulations like HIPAA by monitoring and alerting staff to compliance changes and timelines. This reduces the risk of penalties due to non-compliance. An internal contract manager has to juggle spreadsheets from all payers and government entities, tracking down dates and timelines manually.
- Risk assessment: AI-powered features can identify potential legal issues and compliance risks, protecting organizations from costly liabilities.
5. Enhanced collaboration and visibility
- Cross-functional alignment: Automated contract management systems facilitate collaboration across departments, ensuring that all teams are aligned and informed about contract status and obligations. The contract
- Real-time analytics: The software offers real-time analytics and reporting, providing a clear view of contract performance and enabling timely and data-driven decision-making.
While an internal contract manager can provide personalized oversight, healthcare contract management software offers a more efficient, scalable, and compliant solution.
5 situations when the internal contract manager is the better choice
While healthcare contract management software offers numerous benefits such as efficiency, scalability, and compliance, there are scenarios where using an internal healthcare payer contract manager might be preferable.
- Personalized oversight and control: An internal contract manager that provides personalized oversight and control over contract negotiations and management can be beneficial for organizations that require a high level of customization or specific expertise in handling complex contracts.
- Small-scale operations: For smaller healthcare organizations with fewer contracts, an internal manager suffices to handle the workload without the need for extensive automation. Still, if your organization is closing in on 10 or more payer contracts, the chaos and confusion starts to escalate.
- New technological implementation: No matter how sophisticated your new contract management platform is, it takes a staff member to coordinate implementation. An experienced internal contract manager can handle these processes manually until the organization is ready for full automation. Many contract managers work on a part-time or temporary basis.
- Specialized knowledge: If an organization has unique contract requirements or operates in a niche area, an internal manager with specialized knowledge may be more appropriate for navigating these complexities. You can post a job for a contract manager on the HFMA or MGMA job boards.
- Relationship building: Sometimes the healthcare organization’s priority is to build strong relationships with payers. Internal contract managers can foster strong relationships with payers better than software.
The following situations often call for an internal payer contract manager.
- Transition to Value-Based Care: As the healthcare industry shifts towards value-based payment models, fostering collaborative relationships with payers becomes essential. This collaboration helps align incentives and goals, ensuring both parties work together to improve patient outcomes and reduce costs. Further, in situations where healthcare providers and payers share financial risk through value-based contracts, maintaining a strong relationship is vital. This shared risk incentivizes both parties to work together to reduce costs and improve outcomes.
- Data sharing and interoperability: When the healthcare organization’s priority is to share data optimally with payers, it could take an internal payer contract manager to ensure all systems are connecting. It takes strong, positive payer/provider relationships to optimize care coordination, manage population health, and address health equity challenges. This data exchange helps in making informed decisions and improving patient care.
- Navigating regulatory changes: During periods of significant regulatory changes or healthcare policy updates, strong relationships with payers can help organizations navigate these shifts more effectively. This collaboration ensures compliance and alignment with new requirements.
- Improving patient engagement and outcomes: When healthcare organizations aim to enhance patient engagement and improve health outcomes, collaboration with payers can provide additional resources and support. This includes leveraging payer data and programs to address social determinants of health.
Review our Navigating Payer Relationships post which breaks down when to foster a positive, collaborative relationship and when to take a more assertive, even combative stance with payers.
Ultimately, the decision between using an internal contract manager and software depends on the organization's size, complexity of operations, and specific needs.
Use a healthcare contract management platform that forms the foundation to your revenue
Healthcare organizations face a critical decision when managing contracts: whether to rely on an internal contract manager or leverage a healthcare contract management platform. While an internal manager provides personalized oversight and control, contract management software offers efficiency, scalability, and compliance benefits, automating tasks and reducing operational costs. Your decision depends on your organization’s unique structure, challenges, and opportunities.
MD Clarity’s healthcare contract management platform, RevFind, empowers healthcare providers and organizations by:
- uncovering significant revenue opportunities
- enhancing the evaluation of payer performance
- providing actionable insights that help identify top-performing and underperforming payers
- uncovering data to strengthen your negotiation stance
- modeling the real revenue impact of proposed payer changes
- flagging underpayments
- using predictive analytics to alert staff to claims at greatest denial risk
This comprehensive data serves as a powerful foundation for informed contract negotiations, denial prevention, underpayment identification, and empowered negotiations.
RevFind’s centralized digital repository for all contracts streamlines access and management within a single, user-friendly platform. Its automated alerts for critical contract dates, including expiration, renewal, and termination deadlines ensure your organization meets deadlines.
RevFind’s proactive approach enables healthcare organizations to stay ahead of contract cycles, optimize negotiation strategies, and maintain strong relationships with payers. By leveraging RevFind, healthcare providers can optimize their revenue cycle management, improve financial performance, and focus on delivering high-quality patient care.
Get a demo to see how RevFind can limit your claims reprocessing, raise your net revenue, and put you in control of your contracts.
FAQs
Get paid in full by bringing clarity to your revenue cycle




.avif)
