The profit margin for ophthalmology practices, typically in the ballpark of 30 to 45%, is respectable when compared to other specialties.
Still, recent market forces are shaving ophthalmology revenue, particularly in urban areas where the density of physicians is higher. The push toward digitization is challenging practices dependent on spreadsheets and manual processes. Add the shortage of labor skilled in advanced RCM technologies, and most struggle to optimize ophthalmology revenue cycle management (RCM).
Given these pressures, some ophthalmology practice owners are turning to private-equity-backed management services organizations (MSOs) to help them. The ophthalmologists looking to exit have managed to sell at 5 to 10 times EBITDA.
Twenty years ago, an ophthalmology practice owner sold to a new doctor. That doctor most likely didn’t have a lot of business experience or acumen. But with big buyers steeped in M&A in the waters, books get scrutinized more than ever. The practices that get the highest prices must demonstrate key financial and operational strengths in their Profit and Loss (P&L) statements to secure the highest valuations. Not only must they show consistent revenue growth and stable financial performance over time, they must also show efficient revenue cycle management practices like:
- low claim denial rates, which indicate accurate billing and effective claim follow-up
- quick payment cycles and minimal accounts receivable balances
- reduced bad debt and increased cash flow
Ophthalmology consultant Jeff Nichols writing this month in Cataract and Retroactive Surgery Today foresees that:
“PE interest should continue unabated. This scenario seems likely given the growth in premium IOLs and diagnostic devices and treatments for ocular surface disease.”
MSOs centralize administration to increase efficiency and capital, and even drive much needed modernization.
Even if you’re not looking for a buyer or a partner, there are many benefits in optimizing RCM for ophthalmology. This post tackles the biggest challenges ophthalmologists have in keeping costs to collect under control and improving their revenue. Review how you can address these challenges so that your organization runs efficiently and puts a shine on your P&Ls that impresses lenders, investors, and even buyers.
What is RCM for Ophthalmology?
RCM for ophthalmology is a comprehensive process tailored to manage the financial aspects of ophthalmology practices, ensuring efficient billing, coding, and reimbursement for eye care services. It encompasses a series of steps from patient registration to final payment, aimed at maximizing revenue while minimizing denials and delays.
Effective RCM in ophthalmology involves accurate coding, timely billing, and proactive management of claims denials, all of which are crucial for maintaining cash flow and profitability in ophthalmology practices. By implementing predictable and optimized RCM processes, ophthalmology practices can improve their financial health, which in turn strengthens their ability to provide excellent patient care. This allows staff to focus more on patient care rather than administrative tasks, especially as CMS and private insurers continually adjust reimbursement rules and regulations.
Careful curation of these 10 ophthalmology RCM elements leads to optimized revenue and operations for ophthalmology practices.
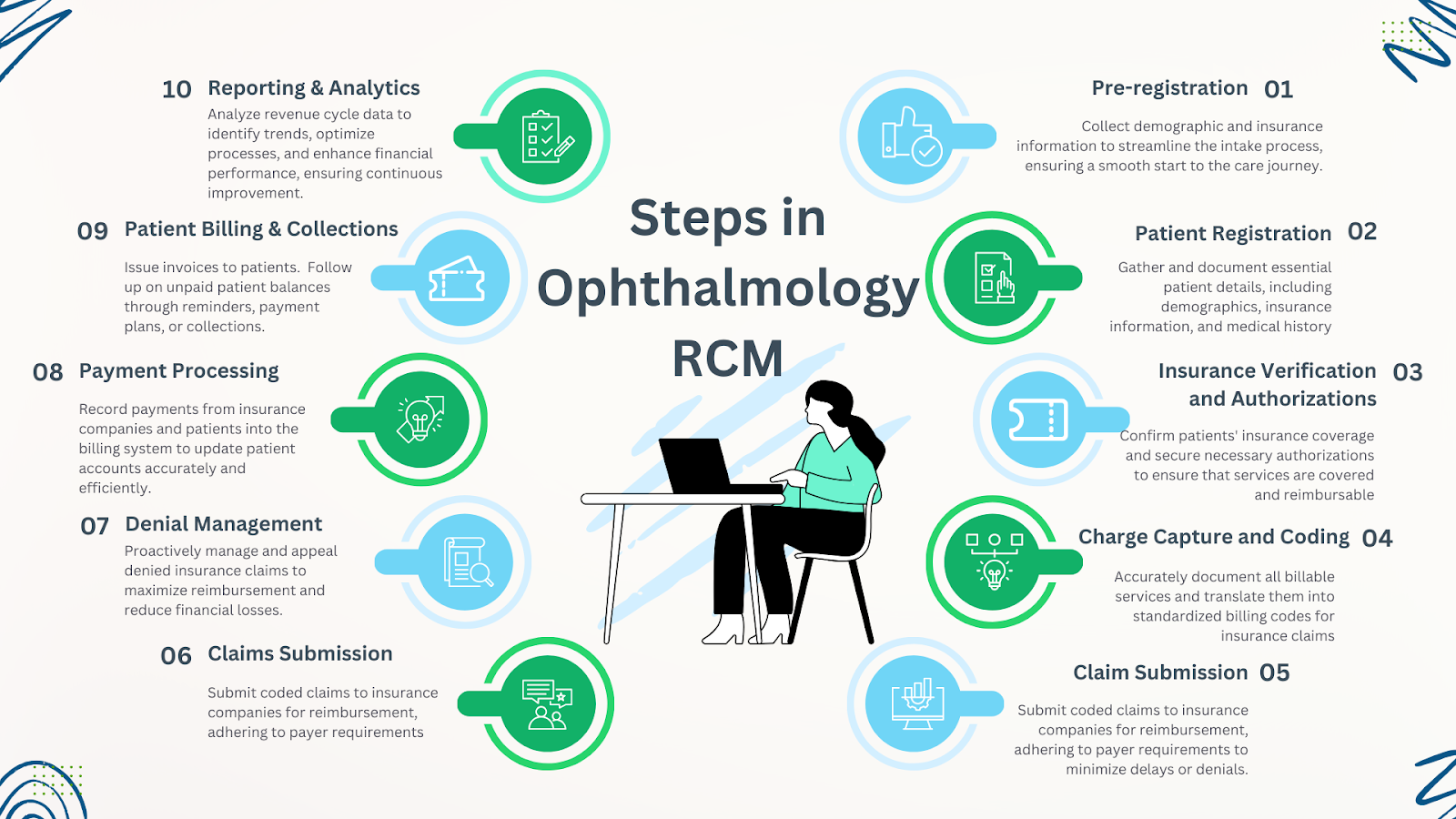
RCM for Ophthalmology: Challenges and Solutions
Where radiology struggles to manage accurate physician referrals and orthopedics has to balance the high cost of treatment with adequate revenue, ophthalmology practices face their own unique challenges in managing their revenue cycle. Review these common challenges, but note their best solutions as well.
Ophthalmology RCM challenge #1: Confusion between medical and vision billing
Ophthalmology patients can present with both medical and vision insurance issues. These patients and even practice staff struggle to understand the difference and which insurance handles which issue.
Often, a patient visits for a routine eye exam, typically covered by vision insurance, but also mentions experiencing dry eyes, a condition that falls under medical insurance. If the billing is not handled correctly, either the vision claim, the medical claim, or both might be denied.
Solution
To ensure accurate billing and avoid claim denials, ophthalmology staff can follow these steps to accurately differentiate between medical and vision insurance:
- Determine the chief complaint: If the visit is for a routine eye exam without medical complaints, bill the vision insurance. If the patient presents with a medical condition like dry eyes, bill the medical insurance.
- Accurate coding and documentation: Ensure that all diagnoses and procedures are accurately documented and coded. Use medical codes for conditions requiring medical treatment and vision codes for routine exams
- Verify insurance coverage: Confirm the patient's insurance coverage before the visit to understand what is covered under each plan.
- Separate billing for combined services: If a routine exam reveals a medical condition, consider billing the medical insurance for the condition and the vision insurance for any routine services not covered by medical insurance.
- Patient communication: Educate patients about the differences between medical and vision insurance and how billing will be handled based on their specific situation.
- Training and updates: Regularly train staff on the latest billing guidelines and insurance policies to ensure compliance and accuracy in billing processes
By following these steps, ophthalmology staff can ensure that claims are submitted correctly, reducing the risk of denials and improving patient satisfaction.
Ophthalmology RCM challenge #2: complex coding and billing combined with higher payer scrutiny leading to high denials
Payers are scrutinizing provider claims more closely than ever.
At the root of revenue-draining denials in ophthalmology is the increasing use of powerful AI solutions by payers to scrutinize claims, particularly those exceeding $5,000. Advanced ophthalmic procedures, such as complex surgeries or specialized treatments, can easily surpass this cost threshold.
AI-driven software meticulously examines claims for even the slightest inaccuracies or missing data. Payers are leveraging this technology not only for initial claim reviews but also to retroactively audit claims they've already approved and paid. The cost of using technology for these reviews is minimal compared to the potential savings for payers. Many leaders in healthcare attribute the rise in payer denials to 15% to the additional work conducted by AI. This heightened scrutiny necessitates that ophthalmology providers ensure claims are flawless before submission, requiring the optimization of the entire revenue cycle.
Fortunately, technology can also benefit providers. RCM software companies often develop solutions for both payers and providers.
Ophthalmology involves intricate procedures requiring precise coding with CPT, ICD-10, and HCPCS codes. Coding errors (e.g., -59 for distinct procedures) can lead to claim denials. When denials get too high, some ophthalmologists invest in specialized coders trained in ophthalmology-specific codes.
The following are tricky spots in ophthalmology coding:
1. Incorrect use of E/M vs. eye codes
Using Evaluation and Management (E/M) codes instead of eye visit codes or vice versa can lead to incorrect billing.
Solution
Ensure documentation supports the chosen code, and select the code with higher reimbursement if both are applicable.
2. Failure to use modifiers correctly
Omitting or misusing modifiers, such as laterality modifiers (-LT, -RT, -25, -50, -78, -79), can result in claim denials. Bilateral eye procedures incorrectly coded as unilateral are common errors that deplete ophthalmology revenue cycle. Incorrect use can mean bundled services that should be paid separately get denied. Also, keep in mind that outdated or incorrect CPT or ICD-10 codes lead to automatic claim rejection.
Solution
Always apply necessary modifiers to indicate distinct services or bilateral procedures.
3. Bundling Errors
Incorrectly bundling or unbundling procedures can lead to underpayment or denials.
Solution
Understand which services are inclusive within a code and use appropriate modifiers for distinct services.
4. Missing or Incomplete Documentation
Insufficient documentation can lead to generic coding and missed reimbursement opportunities.
Solution
Ensure detailed records of diagnoses, treatment plans, and procedures performed.
5. Lack of Specificity in Diagnosis and Procedure Descriptions
Generic coding fails to capture specific components of treatment, leading to missed reimbursement opportunities.
Solution
Ensure specificity in diagnosis and procedure descriptions to maximize reimbursement.
Addressing these common billing errors requires ongoing training, accurate documentation, and often the use of advanced billing and claim scrubbing software, which guides and checks staff work. Still, accurate coding goes a long way in preventing the denials that sap revenue.
Ophthalmology RCM challenge #3: Getting full reimbursements
While denials are a top concern, ophthalmologists often overlook another way to sweep in revenue: underpayment recovery. Focused on denials, RCM staff may ignore when a reimbursement comes in that doesn’t match the rate listed in the contract.
A study in Becker's Hospital Review establishes that providers can face annual losses of 1 to 3% of their net revenue due to underpayments from commercial payers. We’ve worked with physician groups admitting their underpayment rates are as high as 12%, and 7% is not uncommon.
In ophthalmology, reimbursement challenges are a major concern. Ophthalmologists face declining Medicare payments and rising practice costs, which can exacerbate the impact of underpayments. The proposed 2025 Medicare Physician Fee Schedule includes a pay cut, further complicating financial sustainability for ophthalmology practices. Whatever reimbursements are due to them, ophthalmologists should fight for.
Solution
Ophthalmology RCM staff can fight underpayments by manually comparing each reimbursement coming in to the contracted rate, but that means they need to find the contract. With insufficiently skilled staff, too many practices ignore healthcare contract management. We’ve worked with ophthalmology physician groups that hadn’t looked at or updated their contracts in 5 years. One let 12 years go by before revisiting them. Given surging labor and supplies costs, no organization can remain viable without proactively reviewing contracts and demanding higher rates and better terms.
Meticulous contract management defines the terms of service delivery, payment rates, and performance expectations. It is crucial for ensuring financial stability, regulatory compliance, and high-quality patient care.
You can also automate contract management using AI-driven software. This software digitizes and centralizes all agreements in one location. It thoroughly examines each payment against contract terms, identifying any discrepancies for immediate attention. It also enables the comparison of reimbursements with national benchmarks, such as those established by Medicare.
Robust healthcare contract management software also provides the necessary insights to proactively negotiate contracts and guides the process of recovering underpaid funds. Additionally, it helps identify systemic root causes of underpayments, allowing for corrective actions to prevent future discrepancies.
Take a quick, self-guided tour through a powerful contract management and underpayments identification tool:
Ophthalmology RCM challenge #4: patient collections
The healthcare industry is evolving into a new paradigm where patients bear a larger share of their medical expenses. Consequently, patients (often with high-deductible health plans) now contribute significantly to the revenue of ophthalmology practices. According to the Healthcare Financial Management Association (HFMA), patients account for about 30% of provider revenue, marking a substantial increase from previous years.
This shift has led to a rise in lagging accounts receivable, bad debt, and write-offs, which destabilize practices. A recent MGMA Stat poll found that the majority (56%) of medical practice owners reported increases in days in accounts receivable. Furthermore, higher balances are more challenging to collect. Advisory Crowe LLP notes that:
- The collection rate for claims between $5,000 and $7,501 is only about 32%.
- The collection rate for claims between $7,501 and $10,000 is just 17%.
Since ophthalmology often involves higher balances compared to other specialties, practices are particularly reliant on patient payments. Not only must providers secure these funds to ensure financial stability, but they must also educate patients about their financial obligations and payment timelines.
To address this new reality, ophthalmology providers need to develop strategies that enhance patient understanding of their financial responsibilities while intensifying patient collection efforts.
Solutions
Collect more upfront
Assertive upfront collections are becoming essential for ophthalmology groups. Research indicates that the likelihood of securing payment decreases significantly after the patient leaves the healthcare facility. Emphasizing the importance of upfront collections to staff and using compassionate language when discussing patient financial responsibilities can improve outcomes.
Leverage patient payment estimate technology
Patient payment estimate technology supports collection efforts by providing accurate estimates. According to CMS, manually researching insurance EOBs and compiling estimates can take staff up to 1.3 hours. Pre-service patient estimates delivered at the point of service or beforehand help patients plan for their financial obligations. Studies show that patients want to know their healthcare costs upfront: 94% of adults surveyed in a study from Patient Rights Advocate, Inc. and Marist, and 80% in an InstaMed study, prefer to receive this information before receiving care.
Automating eligibility verification and estimate generation can simplify upfront collections. This approach not only streamlines the process but also aligns with patient preferences for transparency in healthcare costs.
Take a quick tour of how you can simplify upfront collections when you automate eligibility verification and estimate generation here:
MD Clarity’s RevFind Fuels Robust RCM for Ophthalmology
Ophthalmology practices face significant revenue cycle management (RCM) challenges, including complex coding and billing, high denial rates, and the need to differentiate between medical and vision insurance claims. Additionally, ophthalmologists must navigate evolving regulatory requirements and payer scrutiny, which demands precise billing and efficient claim management. To address these challenges, practices are turning to advanced RCM solutions that automate billing processes, enhance contract management, and provide actionable insights to improve financial performance and patient satisfaction.
MD Clarity's RevFind solution provides ophthalmology practices with comprehensive visibility into their fee schedules and entire revenue cycle, enhancing financial performance while improving patient experiences. This powerful tool centralizes and digitizes payer contracts, simplifying management and analysis.
RevFind offers several key benefits for ophthalmologists:
- Automated underpayment identification: It automates the comparison of each payment against contract terms, flagging discrepancies and notifying staff to ensure prompt action.
- Contract consolidation and performance monitoring: Contracts are consolidated into a single, accessible platform, making it easier to manage and analyze them. Comparing contracts according to performance and value to your organization gives you leverage during negotiations.
- Benchmarking: Reimbursements are benchmarked against national standards, including Medicare, to ensure fair compensation.
- Proactive negotiations: RevFind delivers critical contract insights to support proactive negotiations, empowering ophthalmologists to secure better rates.
- Underpayment Recovery: It assists in the underpayment recovery process and conducts root cause analysis to maintain accurate reimbursements.
By leveraging RevFind's capabilities, ophthalmology practices can enhance revenue capture by identifying and addressing faulty fee schedule reimbursements promptly. This leads to improved operational efficiency and confident contract negotiations, ultimately securing rate increases that support the financial sustainability of their practices.
Get a demo to see how RevFind optimizes RCM for Ophthalmology.
FAQs
Get paid in full by bringing clarity to your revenue cycle



.svg)
.svg)


