
AI that turns payer complexity into revenue clarity
Centralize, analyze, and enforce payer contracts with AI-native contract management software built for provider organizations.

PayerMonitor
PayerMonitor works alongside your team to interpret payer language, surface key terms, and make contract details easy to find and reference.

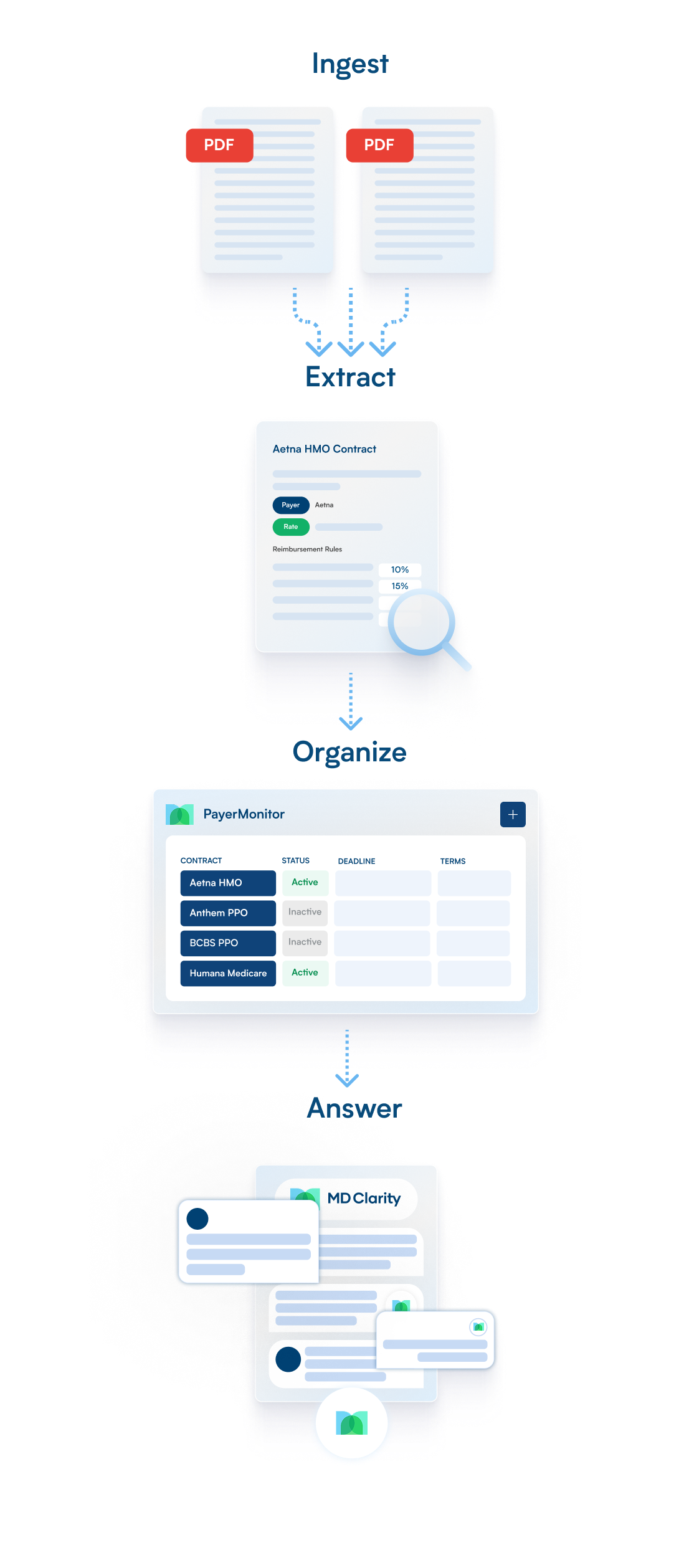
Contracts that work in practice, not just on paper
One system of record unifies all contracts
A single source of truth for contract documents shared across all teams
.svg)
Automated extraction surfaces key terms
Structured reimbursement terms and key dates extracted automatically from every agreement
%20(1).avif)
Every answer comes with a receipt
Fully traceable outputs with citation snippets tied directly back to the original source text
%20(1).avif)
Revenue cycle expertise powers every insight
Expert-trained AI grounded in deep industry knowledge and real provider workflows
.avif)
.svg)
%20(1).avif)
%20(1).avif)
.avif)

Intelligence that drives action for high-performing revenue teams
Intelligence that drives action for high-performing revenue teams
Surface revenue opportunities without manual digging

Accelerate prioritization and response to contract risks

Empower in-house staff with self-service solutions

Intelligence you can explain and trust
We build AI grounded in deep revenue cycle expertise and shaped by real provider workflows. Every output is designed to be reliable, traceable, and transparent.
.svg)
Intelligence you can explain and trust

Security as the baseline

Expertise as the foundation
.svg)
Accountability at every step
.png)
Transparency by design



.svg)
.svg)
.svg)



